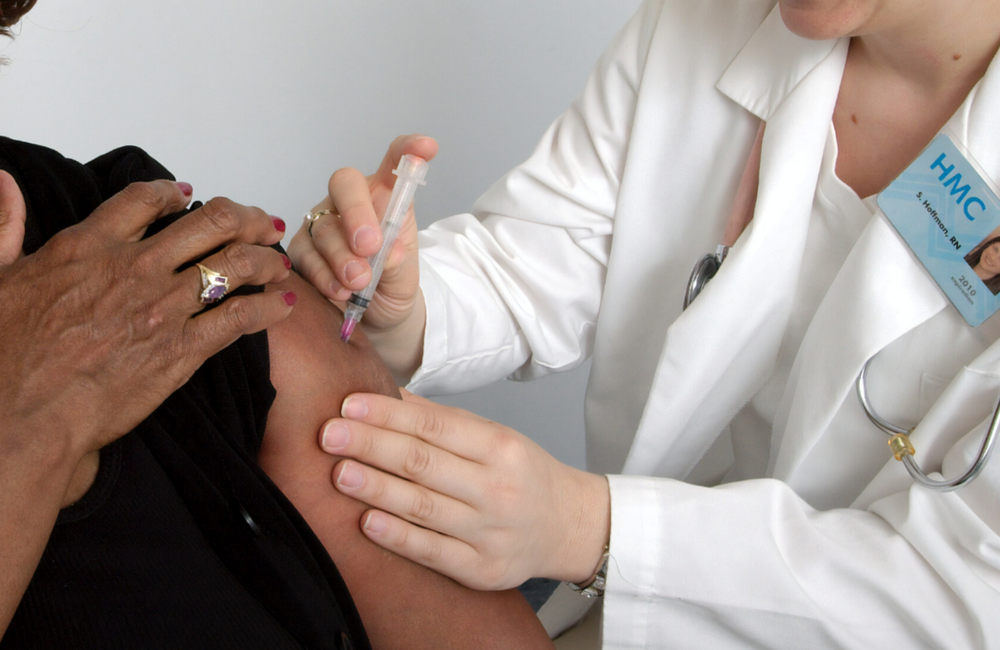
Key Point
Most previous research aimed at producing non-neutralizing antibodies, substances that alert the immune system to destroy invaders. But newer research has focused on inducing broadly neutralizing antibodies that directly kill the virus. Some people use viral vectors to deliver the ingredients inside cells, triggering a stronger immune response. Following their success with COVID-19, mRNA vaccines for HIV are now also being investigated.
We have summarized the history of HIV vaccine trials to date on a separate page.
Two Phase III vaccine trials testing similar vaccines recently ended early due to disappointing results. The vaccines tested delivered a “mosaic” of HIV proteins designed to generate responses against different HIV subtypes. However, the Invocodo trial in African women and the Mosaico trial in gay men and trans women were not tested in August 2021 and 2023, respectively, as neither study found statistically significant efficacy. It was canceled in January. This indicates that scientists need to develop vaccines based on different strategies.
New vaccines are being developed, but so far they are only in Phase I (safety) studies. (See Clinical Trial Stages).
Most of the phase III studies conducted so far aimed to generate so-called non-neutralizing antibody responses.
Antibodies are small protein molecules produced by the billions by the immune system's B cells when they detect a foreign invader. Those molecules can adapt to match the features of an intruder's surface, such as a lock or key.
Non-neutralizing antibodies do not directly destroy the invader, but alert other parts of the immune system, such as CD8 cells, to enter and destroy the invader.
Neutralizing antibodies can directly kill invaders. One type of vaccine under consideration is designed to stimulate the production of so-called broadly neutralizing antibodies (bNAbs).
Although these occur naturally during chronic HIV infection in a small number of people, it is too late to have any protective effect. They have unusual characteristics that allow them to penetrate HIV's sugar molecule coat and disable the molecular “tools” that HIV uses to enter cells.
bNAbs are already being studied as drugs given as an intravenous drip to treat HIV and as a type of PrEP. But getting the immune system to start producing bNAbs prior to HIV infection is a much bigger challenge.
It involves figuring out what types of cells can produce bNAbs in the first place, and then using molecular probes (which are very rare) to look for them in the body. Repeated administration of vaccines designed to stimulate them may produce more cells capable of producing bNAbs. This Scripps Research Institute vaccine is an example of this approach.
Glossary
vaccine
A substance containing antigenic components from infectious microorganisms. By stimulating an immune response (not disease), it may protect against subsequent infection by that microorganism or induce an immune response against an established infection or cancer.
Broadly neutralizing antibodies (bNAbs)
Neutralizing antibodies (NAbs) are antibodies that completely protect target cells from antigens. Broadly neutralizing antibodies (bNAbs) are neutralizing antibodies that have this effect against a wide range of antigens. A large number of broadly neutralizing antibodies have been isolated from people living with HIV. Some of them are being studied and, in some cases, being used in clinical trials to protect humans from HIV infection, treat HIV infection, and kill HIV-infected CD4+ T cells in latent carriers.
trial
A clinical trial is a research study that evaluates a treatment or intervention in human volunteers to answer specific questions about safety, effectiveness, and medical effectiveness.
antibody
Protein substances (immunoglobulins) produced by the immune system in response to foreign organisms. Many diagnostic tests for HIV detect the presence of antibodies to HIV in the blood.
Other vaccine researchers believe it's worth revisiting another arm of the immune system: T cells (CD8 cells), which kill cells infected by viruses. After all, this is the only natural response proven to suppress HIV infection in elite management.
The failed STEP trial aimed to induce a CD8 response. Researchers now understand why the vaccine made some people more vulnerable to HIV infection, and say such outcomes can be avoided. They also devised a vaccine containing far more different HIV antigens. The Jenner/Oxford University HIV-CORE 0052 and 006 vaccines are examples.
A more innovative type of T-cell vaccine involves the use of so-called replicating vectors.
Vectors are used in many HIV vaccines, including RV144 and its successors, and indeed in other vaccines such as the Oxford/AstraZeneca COVID vaccine. A vector is a “shell” of a virus that causes asymptomatic or very mild disease in humans and is used to contain the active ingredient, her HIV antigen. Vectors are much better at getting into cells than vaccines like AIDSVAX, which consist only of naked HIV DNA or proteins.
Most vectors are designed to enter cells only once and are unable to replicate and cause ongoing infection. Replicating vectors, on the other hand, replicate similar to a viral infection, thereby spreading HIV vaccine antigens throughout the immune system and inducing a deeper and broader immune response. Back in 2013, one vaccine based on cytomegalovirus (CMV), a ubiquitous virus that is usually asymptomatic, completely eliminated HIV from 50% of a group of monkeys that were already infected. When, it caused excitement. Studies have shown that a particularly deep and diverse CD8 response is elicited.
Human trials of CMV vaccines have taken a long time because the deliberate introduction of replication-competent virus raises obvious safety concerns. However, a phase 1 clinical trial of a human CMV vaccine, VIR-1111, is currently underway.
This is just one example of the current approach. Other HIV vaccines use RNA technology, which was used to make the highly effective Pfizer and Moderna coronavirus vaccines.